Rate of Uninsured Kids Increased Nationwide and in 29 States in 2024
After Years of Progress, Uninsured Rates are Rising for Children Nationwide

The latest data from the Census Bureau’s American Community Survey show that the U.S. rate of uninsured children increased to 6% in 2024, after holding at 5% for three years in a row. More than half of the states and D.C. saw their rates rise, as well. Nationwide, this equates to nearly 4.7 million kids under age 19 lacking insurance coverage in 2024, an increase of about 500,000 from 2023, largely due to expired pandemic-relief measures. Experts project these numbers will continue to rise. Whether uninsured rates trend up or down, large disparities persist by children’s race and ethnicity, immigration status, age and geography, highlighting our country’s inequitable access to health coverage that must be addressed.
How the Pandemic Affected Coverage
After the COVID-19 pandemic hit, Congress passed multiple relief measures that bolstered the insurance safety net for children and families, including:
- increased state funding for Medicaid and continuous coverage protection to keep states from disenrolling people until April 1, 2023;
- reduced costs for purchasing coverage through the Affordable Care Act (ACA) health insurance marketplace and expanded enrollment periods and outreach; and
- expanded federal and state measures, such as the Children’s Health Insurance Program (CHIP), to improve access to insurance.
These policy efforts helped low-income families weather the pandemic’s economic crisis and contributed to the low 5% uninsured rate for kids from 2021 to 2023. However, after pandemic protections expired in early 2023, the number of uninsured Americans began to climb — and by Sept. 2025, an estimated 17.3 million individuals had lost Medicaid/CHIP coverage, according to the Kaiser Family Foundation.
Additional legislative changes in 2025 have led the Congressional Budget Office and others to project a continued rise in individuals without health coverage.
What Are Medicaid and CHIP?
Increased enrollment in Medicaid and CHIP was behind the reduced U.S. rate of uninsured children during 2021–2023, but what do these programs entail?
- Medicaid is a large public health insurance program for children and adults who meet a low-income eligibility threshold. It covers almost 4 in 10 kids nationwide. Under the ACA, states can expand Medicaid eligibility to more low-income families. In Sept. 2025, all but 10 states had expanded their Medicaid eligibility requirements.
- CHIP is another public insurance program for children in families whose incomes are too high to qualify for Medicaid but likely too low to afford private insurance.
- While kids and young adults can be covered under a parent’s or guardian’s insurance plan up to age 26, only children under age 19 can qualify for Medicaid or CHIP.
Nearly Two in Five Kids Are Covered by Public Insurance
Nationwide, 38% of children were covered by public health insurance in 2024, including 33% who relied on it as their only source of coverage and 5% who had a mix of public and private insurance. Nearly half (48%) of kids were covered through employer-based insurance that year, while far fewer children had either a plan purchased directly from an insurance company (6%) or other private insurance (2%).
At the state level in 2024, the share of kids who rely on public insurance ranged from 13% in Utah to more than half (53%) in New Mexico.
Why Insuring Children Matters
Kids with insurance are more likely to access timely medical care for health needs. They have improved physical, mental and behavioral health outcomes compared to those without coverage. Poor health during childhood can affect virtually every area of a child’s life, including school performance, and it can have lasting consequences into adulthood on their health, well-being and financial security.
Children eligible for public insurance are especially likely to see the benefits of health coverage, including increased economic stability for their families. For instance, when a family receives Medicaid, they can use more of their income on other basic needs like food and housing. Medicaid has also been linked to reduced medical debt and bankruptcies, and it is considered one of the nation’s leading anti-poverty programs.
Insuring parents helps children in other ways, too. It increases the likelihood of parental physical and mental health, strengthens parents’ ability to care for their children and improves infant health, child health and school outcomes.
Children’s Risk of Being Uninsured Varies Substantially by State
Differences in state policies and practices, as well as local economic conditions, largely influence the variation in access to coverage across the country. In 2024, 17 states exceeded the national rate of uninsured children, with figures of 7% or higher, according to the KIDS COUNT Data Center. Most of these states were in the Southern and Western regions of the country. The Northeast states of Massachusetts and New Hampshire had the lowest uninsured rates for kids (both 2%) in 2024, while Texas continues to have the highest rate, with 14% — or 1.1 million kids — lacking insurance.
Children Age 18 and Below Without Health Insurance in United States (2024)
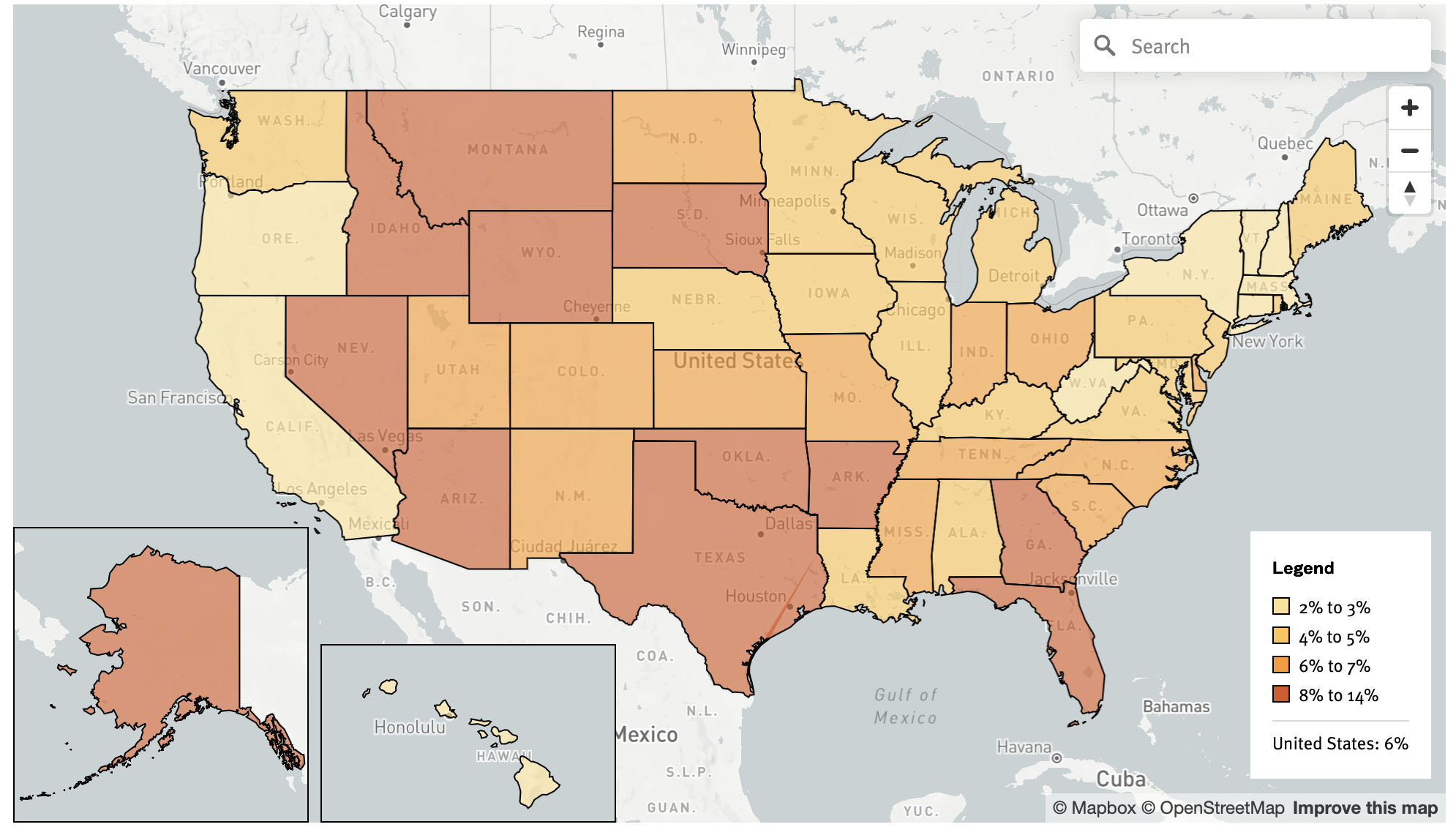
From 2023 to 2024, the children’s uninsured rate increased in 29 states and D.C., from one to three percentage points. Nearly all other state rates remained flat in this period.
Inequities Persist, Particularly for American Indian and Alaska Native Children
The rate of uninsured American Indian or Alaska Native children (12% in 2024) has been at least twice the national average in all seven years of data available on the KIDS COUNT Data Center, and the rate for these kids worsened by one percentage point in 2024. The uninsured rate for Latino children has also remained higher than the national level for seven years and inched up over the last two years, reaching 10% in 2024. Black children saw increases in the last two years as well, from 4% of kids without insurance in 2022 to 6% in 2024. Rates for multiracial children have been slightly above the national average in recent years and increased by one percentage point in 2024, to 7%. For the last seven years, figures for white and Asian and Pacific Islander kids have remained even at 4%.
In addition, immigrant children, particularly those who are undocumented, are at increased risk of being uninsured and having difficulty getting medical care, compared to their peers with U.S. citizenship. The Census Bureau reported that more than 1 in 5 (22%) non-citizen children were uninsured in 2024, similar to 2023. Figures were nearly as high for foreign-born kids as a whole, regardless of citizenship. Among non-citizen children who have lived in the country less than five years, uninsured rates jump to 29%, according to a 2023 analysis by the Kaiser Family Foundation.
Teens and young adults are vulnerable, too. The Census Bureau reports that 14% of young adults ages 19 to 25 lacked health insurance in 2024, the highest rate of any age group. Teens are also more likely than younger children to lack coverage. The KIDS COUNT Data Center tracks health insurance status for youth and young adults ages 14 to 24 and reports that 11% of these young people did not have health insurance from 2019–2023. This rate is double (22%) for American Indian or Alaska Native youth and young adults and more than 1.5 times the national rate for Latino youth (18%).
Addressing Inequities and Barriers to Health Insurance
Millions of children, young adults and parents lack health insurance — and the number of uninsured Americans is projected to rise — while concerning disparities in access to coverage remain. Concerted action is needed to ensure that all children and families can obtain affordable health insurance and medical care. Many states are taking action and more can be done, such as keeping eligible families enrolled in Medicaid, helping them enroll in other plans and/or offering state-based subsidies for marketplace enrollees. Federal lawmakers can also take steps to make coverage more affordable and accessible for low-income families.
Policymakers and leaders in multiple sectors must continue working toward systemic change to address the long-standing inequities and barriers that contribute to the disproportionately high uninsured rates among American Indian or Alaska Native and Latino children. Additionally, leaders can remove barriers for immigrant families to enroll in Medicaid and the ACA health insurance marketplace, and support strategies to increase enrollment among young adults. Leaders at all levels can take steps to simplify the system and improve access to coverage, particularly for the most vulnerable populations.
More Child and Family Health Resources
See all health insurance data on the KIDS COUNT Data Center, including these recently updated indicators:
- State Map of Children Under Age 19 Without Health Insurance
- Children Without Health Insurance by Race and Ethnicity
- Children With Coverage by Type of Health Insurance
- Youth and Young Adults Ages 14 to 24 With Health Insurance
Additional resources:
- Tips for Tapping Medicaid for Youth with Justice Involvement, 2024
- COVID-19 Survey: Insights for Policymakers on Supporting Families, 2022
- KIDS COUNT Data Book
Sign up for the Foundation’s newsletters to get the latest data, reports and resources






